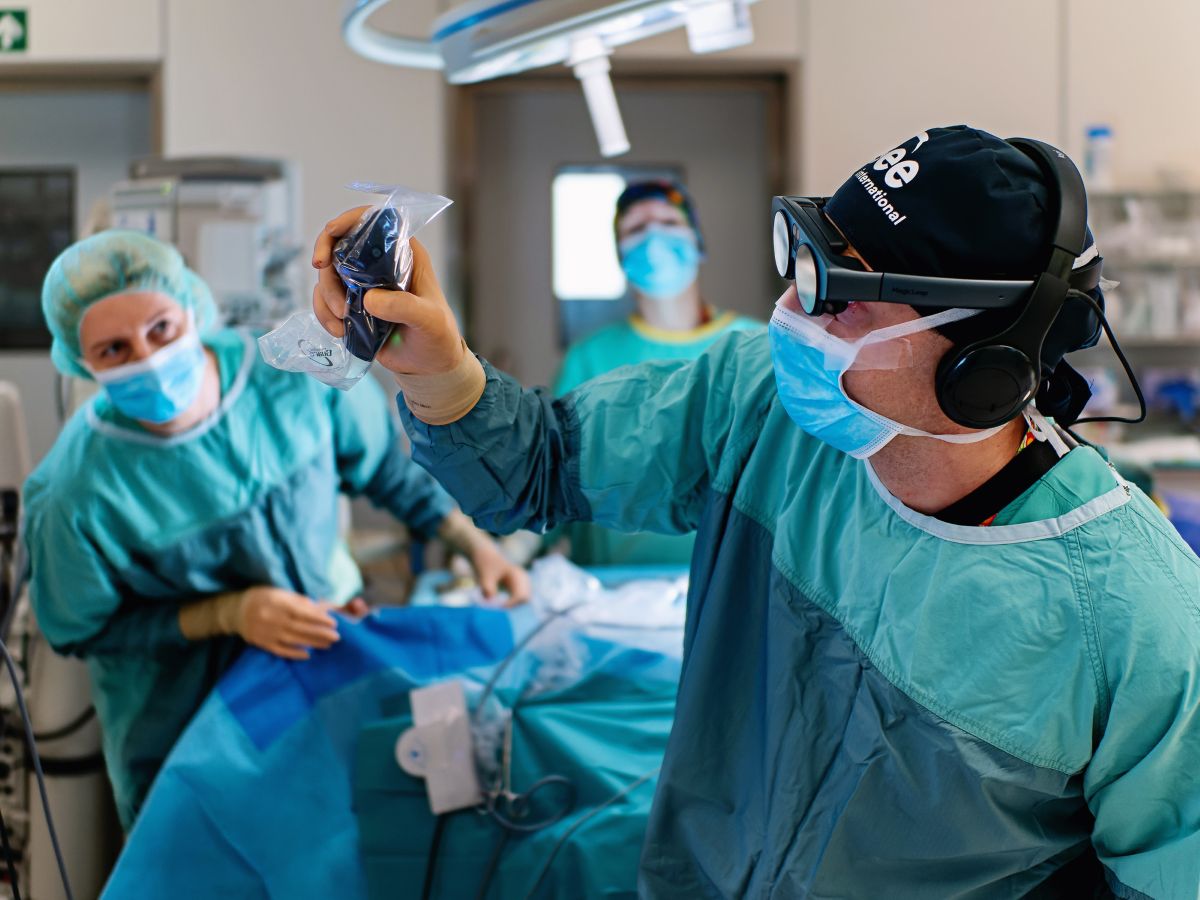
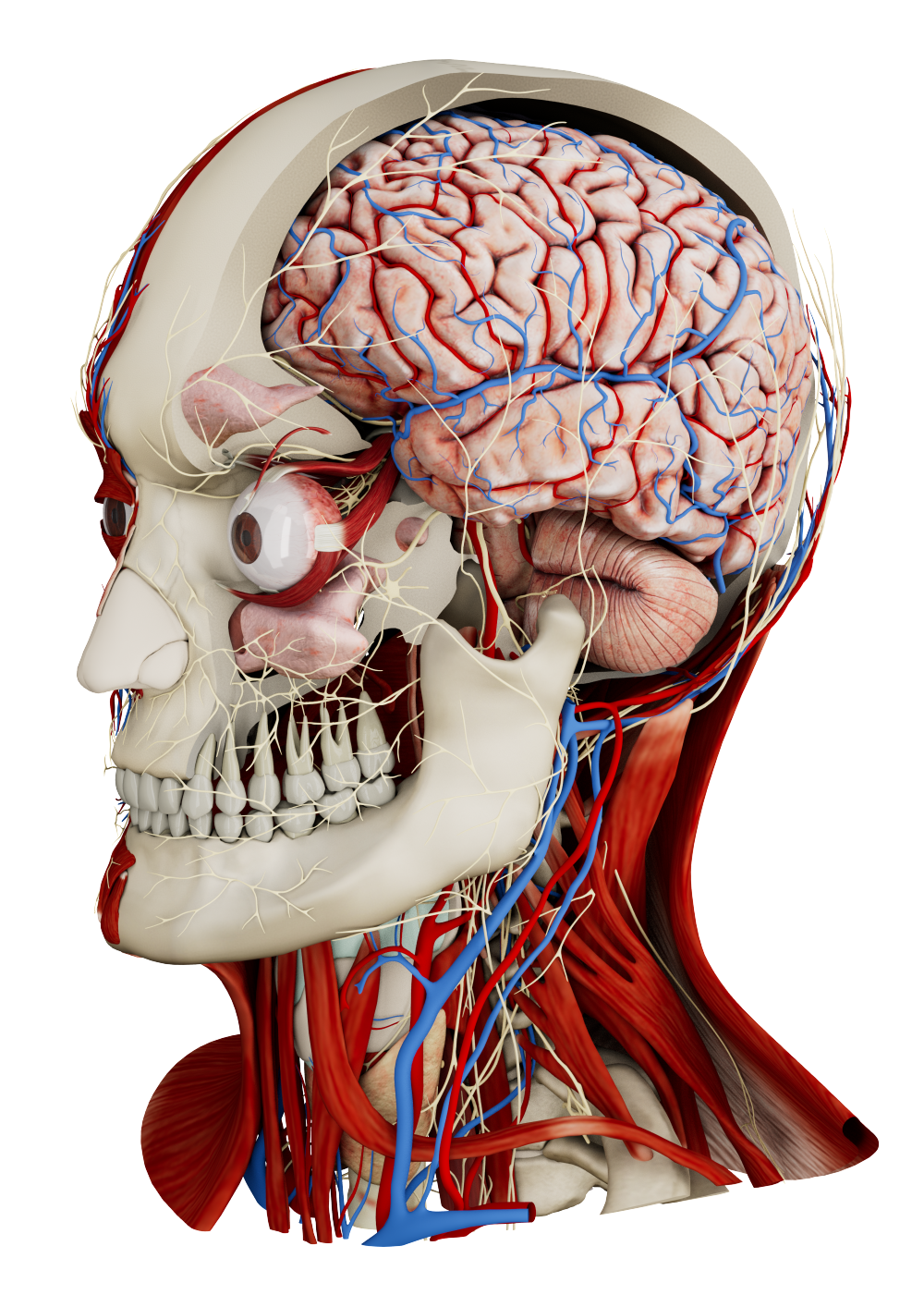
Oncology presents some of the most demanding challenges in medicine. Tumors often arise in anatomically delicate regions, treatment planning demands millimeter-level precision, and management decisions frequently require coordination across large multidisciplinary teams. Immersive technologies such as spatial imaging and automatic segmentation address these challenges by bringing patient-specific data into interactive 3D space. Not only do these advancements promise to improve surgical precision and treatment planning but also enhance patient education, and support efficient decision-making across the cancer care continuum.
Important notice regarding surgical planning and professional clinical use
Specialized functionalities for surgical planning and pre-operative professional applications are exclusive to Medical Imaging XR PRO FDA. This version is not yet available. Information about the release date will be published here soon.
Medicalholodeck is currently undergoing the required FDA (U.S. Food and Drug Administration) and CE (Conformité Européenne) certification processes. Our team is working diligently to ensure full compliance with all regulatory standards, and we expect Medical Imaging XR PRO to be available in both the United States and the European Union soon.
For updates on product releases, regulatory progress, and availability, or for any related inquiries, please contact info@medicalholodeck.com.
Patient information
The complexity of oncological conditions may negatively impact patients and caregivers’ comprehension of their diseases, often leading to anxiety and low engagement in treatment. Immersive VR helps bridge this gap by turning 2D imaging data into intuitive, navigable 3D views. Patients report that VR makes tumor size, location, and surrounding anatomy easier to understand, which increases confidence, reduces fear, and encourages more active participation in their care.
Neuro-oncological surgery
Brazilian surgeons reported using augmented reality overlays intraoperatively for a series of intracranial tumor resections. Their case series described multiple patients harboring diverse intracranial tumors, including diffuse gliomas and glioneuronal lesions. The patients underwent AR-assisted surgeries, where virtual surgical plans were registered and projected onto their anatomy in real time.
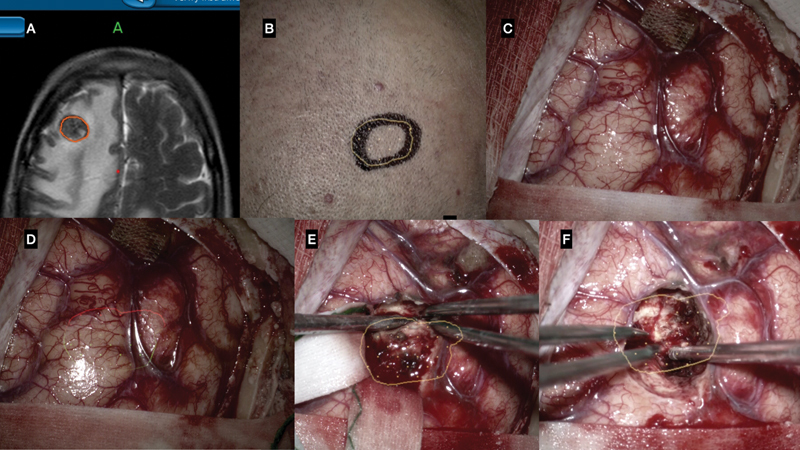
Augmented reality (AR) neuronavigation system for computer-assisted volumetric resection of subcortical tumor. ( A ) Surgical planning (StealthStation S7 Surgical Navigation System) delineating tumor (red). ( B ) Augmented reality holographic projection for guided craniotomy and incision. ( C ) Surgical field without AR hologram projection. ( D ) Surgical field with AR hologram projection of the tumor (yellow and red). ( E ) Microsurgical resection guided by holographic projection (tumor: yellow). ( F ) Complete resection confirmed by holographic projection.
During the procedures, the AR overlays aided in planning skin incisions, craniotomy boundaries, and guidance on tumor localization and extent. The system allowed surgeons to visualize tumor margins projected onto cortical surfaces and to adjust resection trajectories accordingly.
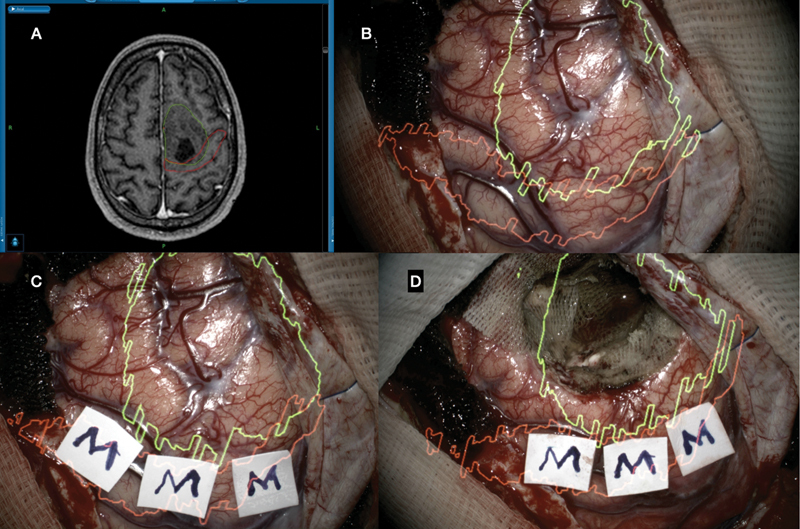
Augmented reality (AR) neuronavigation system for computer-assisted volumetric resection of left frontal tumor adjacent to the motor area. ( A ) Surgical planning (StealthStation S7 Surgical Navigation System), delineating tumor (green) and motor cortex (red). ( B ) Surgical field with augmented reality hologram projection (tumor: green and cortex motor: red). ( C ) Brain mapping confirming the position of the motor cortex, corresponding to the holographic projection of the cortex motor (red). ( D ) Microsurgical resection guided by cerebral mapping and augmented reality.
AI-segmented lung cancer
The integration of Artificial Intelligence in thoracic procedures, including segmentectomies or lobectomies commonly used in cancer treatment, holds significant potential to enhance surgical precision and safety. A system combining AI-driven segmentation with 3D data visualization in augmented reality was shown to be valuable for intraoperative guidance during robotic-assisted lobectomies. The AI technology automatically identified key thoracic structures, including the pulmonary artery, pulmonary vein, lobes, and airways, from patient imaging data, and enabled the resulting 3D models to be overlaid onto the surgical field in real time. This augmented reality visualization allowed surgeons to track and navigate critical anatomy with greater accuracy throughout the procedure.
MR in colorectal cancer treatment
Right hemicolectomy is a common surgical procedure for the treatment of colorectal cancer, one of the most prevalent cancer types. Despite its frequency, complication rates and postoperative mortality highlight considerable potential for procedural improvements.
The mixed reality technology enabled surgeons to interact with 3D patient data during D3 lymph node dissections. The holograms could be scaled and rotated to align with the laparoscopic monitor, allowing precise visualization and verification of vascular anatomy, including the superior mesenteric artery and vein.
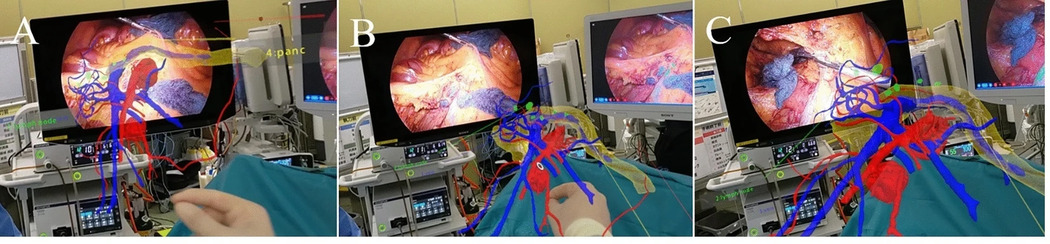
(A) A video recording of the surgeon’s view. A 3D hologram can be placed next to the laparoscopic monitor at any size and angle. Lymph node dissection in front of the superior mesenteric vein (SMV) during laparoscopic right hemicolectomy. (B) The angle of the 3D hologram is adjusted using the SMV as a landmark. (C) The right colic artery is dissected while the anatomy is confirmed via a 3D hologram.
Compared to the conventional surgeries, the MR-assisted procedures resulted in lower blood loss and shorter postoperative hospital stay. Surgeons also reported treating a greater number of vessels and harvesting more lymph nodes around the middle colic artery and vein.
Tumor board discussions
Virtual reality shows promise in enhancing decision-making during multidisciplinary tumor boards. Traditionally, these meetings, bringing together oncologists, radiologists, and surgeons, rely on 2D imaging and the individual expertise of participants. VR introduces a more collaborative and immersive approach, enabling teams to analyze 3D patient data in a shared virtual environment. This facilitates clearer communication, deeper understanding of clinical cases, and more efficient, evidence-based decision-making.
The integration of immersive technologies into oncology, from surgical planning and intraoperative guidance to education and multidisciplinary coordination, demonstrates how digital innovation can bridge gaps between data and decision-making, leading to improved diagnostic precision and surgical accuracy. As these tools mature, they are bound to make cancer care more personalized and accessible.
How to get started
Medicalholodeck integrates with secure hospital systems, providing PACS access, HIPAA-compliant data handling, and full patient data security. It runs on stereoscopic 3D displays, VR headsets, mobile devices, and standard Windows systems, enabling flexible use in hospitals, classrooms, and training centers.
Specialized features for surgical planning are exclusive to Medical Imaging XR PRO. Currently, Medicalholodeck is available only for educational use. The platform is undergoing FDA and CE certification, and we expect Medical Imaging XR PRO to be available soon in the U.S. and EU markets.
For updates, regulatory news, availability, or questions contact info@medicalholodeck.com.